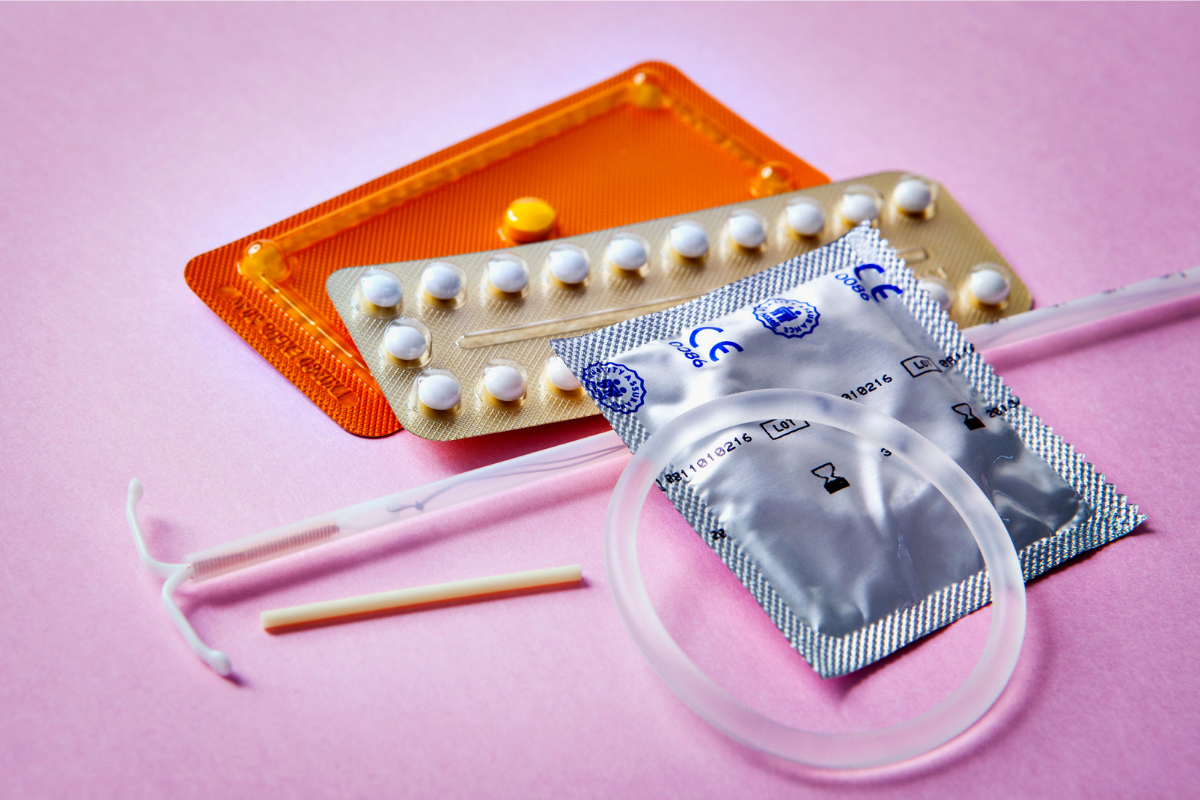

Birth Control
Wondering which method is right for you? Learn about available birth control methods here.


There are a lot of different types of birth control to choose from. We know that can choosing a method can feel hard or overwhelming--and want to help you make an informed, confident decision about a method that feels right for you.
Below is a quick review of the different methods along with several resources where you can find out more. While there are multiple options for preventing pregnancy, it’s important to remember to use latex or polyurethane condoms to reduce the risk of sexually transmitted infections (STIs).
It’s best to talk to a healthcare provider you trust about your birth control options. If you do not have one, or don’t have insurance, you can find a provider in your area in our Find A Clinic tool.
Long Acting Reversible Contraceptive (LARC)
Long Acting Reversible Contraceptives (LARCs) are birth control methods that are inserted by a medical professional and offer long term protection. These LARC methods include Intrauterine Devices (IUDs) and hormonal implants.

Intrauterine Devices (IUD)
IUDs are a small T-shaped device that are placed in the uterus by a medical professional like a doctor or nurse. They last for 5-12 years depending on the type. There are many IUDs that use hormones and one, Paragard, that does not and uses copper instead. Paragard can also be used as emergency contraception. Some IUD users report their period becoming much lighter and sometimes stopping altogether.
An IUD can also offer privacy, because most people won’t be able to tell you have an IUD. Sometimes partners do report being able to feel the strings of the IUD. If you want to conceal that you have an IUD from your partner, discuss options of cutting the strings shorter with your healthcare provider. An IUD must be removed by a medical professional, but once it’s removed you can become pregnant soon after. An IUD is one of the most effective non-permanent forms of preventing pregnancy.

Hormonal Implant
Also very effective is the hormonal implant. It is about the size of a match stick and must be implanted by a medical professional just below the skin in your upper arm.
Implants also require a medical professional to remove the device when it has reached its term or when you decide to no longer use it.
Hormonal Contraception
Other birth control options include birth control pills, the shot, the patch, or the ring. All of these options are hormonal methods but vary in the type of hormones they use.

The Pill
The birth control pill has been around for a long time and there are a wide variety of birth control pills available. You take it once a day, every day. They must be taken every day to be effective. Skipping a pill can lead to unexpected pregnancy.
The Shot
The shot, also known as "Depo," is a shot injected into the arm every three months by a healthcare worker.
The shot contains a hormone called progestin that prevents eggs from being released from the ovaries. It also causes cervical mucus to thicken, making it harder for sperm to reach an egg.

The Ring
The ring is a small, flexible plastic ring that you manually place inside the vagina and leave there for 3-4 weeks. After 3-4 weeks, you discard the old ring and place a new one.
A new ring, Annovera, that lasts for up to a year has recently become available and can be easily inserted and removed by the user.
The ring is infused with hormones that slowly release into your body, preventing the ovaries from releasing eggs.

The Patch
The patch is a small, thin piece of plastic that is placed on the body like a sticker and replaced once a week.
The patch is infused with hormones that enter the body through the skin.
Non-Hormonal Methods
There are other birth control methods that are both short term and don’t involve hormones. These include condoms (both internal and external), sponges, fertility awareness-based methods, and spermicides. These methods are less effective at preventing pregnancy, but may be the best fit with a person's preferences and personal reproductive life goals. Many of these methods, like condoms and spermicide, can be purchased at a local pharmacy and don’t require a medical appointment to access. However, you'll need to make an appointment with a healthcare provider for a diaphragm.

Condoms
There are two kinds of condoms – external and internal.
External condoms are often what people think of first when they picture a condom – it comes in a little foil packet and goes over an erect penis.
Condoms come in several shapes, textures, and materials. Latex condoms, when used correctly, are your best option for preventing some sexually transmitted infections (STI) like chlamydia, gonorrhea, and HIV.
Internal condoms are designed to be worn inside the vagina for preventing pregnancy or inside the vagina or anus to prevent STI.

Sponges
Sponges are small and made of a plastic foam that’s worn inside the vagina.
Sponges release spermicide, a chemical that stops sperm from moving before they can cause a pregnancy.
A sponge can be inserted up to 24 hours before sex, but a new sponge should be used every time you have sex to prevent pregnancy.

Diaphragms
Diaphragms are small silicone cups a few inches across.
They're inserted into the vagina with spermicide before sex and worn during sex. They cover the cervix and block sperm from entering it.

Spermicides
Spermicides come in many forms – creams, gels, films, etc. – and are inserted in the vagina before sex.
Spermicide is a chemical that stops sperm from being able to move. This keeps them from being able to reach an egg to cause a pregnancy.

Fertility Awareness Based Methods
Also called Natural Family Planning, Fertility Awareness Based Methods (FABM), rely on the user to track menstrual cycles and other clues in the body about when they are fertile and to avoid unprotected sex during that time.
There are several methods for tracking day-to-day fertility including counting days since last period, measuring body temperature, and checking and tracking cervical mucus.

Abstinence
Abstinence means different things to different people--and may mean different things to you and your partner. For birth control, abstinence means not allowing sperm near the vagina--or no vaginal sex. For STI prevention, abstinence means no genital-to-genital or mouth-to-genital contact--or no vaginal, anal, or oral sex. If abstinence is a method you and your partner are considering, take some time to talk about what abstinence means to each of you.
Emergency Contraception

Emergency contraception (EC) can stop a pregnancy before it starts, if taken after someone who can get pregnant has unprotected sex. While a Paragard IUD can be used as EC, most EC comes as a one pill dose. Some EC can be used up to five days after sex to prevent pregnancy, others can only be used up to three days after sex. Be sure to discuss this with your pharmacist or healthcare provider for which kind is best for you. You can purchase EC over the counter at most pharmacies and from some health clinics.
Permanent Birth Control

Thinking about a permanent birth control option?
For people with ovaries, sterilization (or tubal ligation) closes or blocks the fallopian tubes--preventing an egg from meeting sperm.
For people with testes, sterilization (or vasectomy) prevents sperm from being released. A healthcare provider can discuss permanent birth control options with you.
Choosing a Method
Figuring out what method may be best for you depends on what your personal reproductive life goals are for the future. If you are interested in beginning or changing your method, talk with a medical provider you trust about what is most important to you in your birth control method and which option will fit you best. If you do not have insurance or need assistance getting birth control, you can find a low-cost provider at our Find a Clinic tool.
More resources on birth control
Here are some other helpful place to learn more about your birth control options and the different methods.
Sign Up for Email Updates
Join us as we work to bring high-quality sexual and reproductive healthcare to everybody in Texas.


